By : Viren Shetty, Director and SVP of Strategy at Narayana Hrudayalaya Ltd
In 1936, Columbia sociology Professor Robert K Merton published a seminal paper entitled, “The Unanticipated Consequences of Purposive Social Action”. He wrote about the ‘imperious immediacy of interest’, in which government legislation that desperately seeks one outcome, wilfully ignores the unintended consequences of that action. The most famous example of unintended consequences is the US Food & Drug Administration – which has a backlog of several years’ worth of new drug approvals. The FDA, originally created to protect consumers has, through its own inefficiency, killed thousands of people waiting for those lifesaving medications, and raised the costs of drug discovery for billions of people around the world.
In 2016, the government of Karnataka created a committee of health experts chaired by retired Chief Justice Vikramajit Sen to propose amendments to the Karnataka Private Medical Establishments Act of 2007, with the hope of reducing healthcare costs for patients. On the 13th of June, the government tabled a bill before the Karnataka Assembly that bore little resemblance to the Justice Sen proposal. Two key provisions of the bill will make the biggest impact have on the future of healthcare in Karnataka. These are – “It is considered necessary to … have effective control over Private Medical Establishments”[1], and “Every Private Medical Establishment shall follow the rates as fixed by the Government”[2].
There are a host of other amendments that will reduce the freedom of doctors to manage their own establishment, increase penalties for violations, reduce the duration of licenses, but I won’t focus on those. I also won’t delve into the hypocrisy of not holding government hospitals to the same standard as private hospitals. I will focus instead on the unintended consequences of two main objectives of this bill – Increased Regulatory Burden and Price Control. I argue that this will raise prices for patients over the long run, reduce their choice of provider, and lower the quality of healthcare that they receive.
First of all, I applaud the noble objectives of this bill. It will encrust a first-world regulatory structure on top of our inadequate third-world infrastructure. Since the public believes that doctors are not to be trusted, the government will create multiple layers of oversight through ad-hoc inspection committees. These committees will be able to define the standards of infrastructure, staffing levels, or “any other function”. These same committees will have the right to inspect every single department of the hospital. And because the government believes in efficiency, the same committees will also have the power of a civil court, thus playing the role of judge, jury and executioner.
I shall choose to believe that this new cadre of inspectors will discharge their functions honestly and will not, repeat not, invoke their power to arrest any hospital owner on arbitrary non-compliance charges for six months to three years[3] as a means to seek rents. I shall instead focus on the rising costs of compliance, highlighted brilliantly by William Baumol in his theory of cost disease[4]. He showed that over time, technological progress lowers the costs of manufactured goods, but the costs of labour-intensive services like healthcare and education increase, often far in excess of wage inflation. There are many reasons, but the most important one is when companies have to hire an army of people to deal with the compliance issues generated by overzealous regulation.
Most private healthcare in India is delivered through individual practitioners and small nursing homes. These mom-and-pop establishments operate with low margins, collect cash, pay no taxes and make do with low overheads. The facilities they operate in wouldn’t pass an NABH[5] audit but they serve a valuable role in the delivery of affordable secondary care, especially in small towns. There’s no way they can afford the software needed to track clinical outcomes, nor pay for quality control specialists. When the inspectors come, they will have to make a choice between spending money they don’t have on facility upgrades or simply closing down. There’s a third choice, but I’m confident that no reasonable person would even dream of asking the honest inspector to overlook the non-compliances in exchange for some kind of, (gasp) benefit. The nursing homes that end up spending money on electronic medical records, ETO sterilizers, finance managers, fire protection, auditors, will survive, but all those additional overheads will be borne by, you guessed it, the patients. The tragedy in all of this, is that the facilities that are best equipped to handle these regulations are those old rascals – large multispecialty hospital groups. They will benefit the most when the government eliminates their competition – small nursing homes and private practitioners. Remember, regulation always raises barriers to entry and incumbents benefit most from regulation.
Finally, I will delve into the role that price control will play in raising overall costs and lowering overall quality in healthcare. Public health activists choose to ignore decades of research[6] that show price controls don’t work, and so shall I. Instead, I will share a slice of reality.
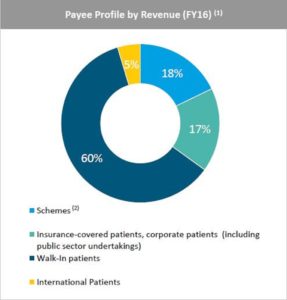
Source: Narayana Hrudayalaya FY 16-17 investor presentation
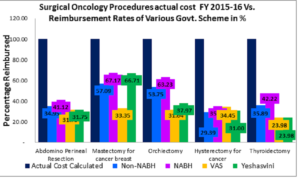
The chart above shows the revenue mix for different categories of patients that walk into my hospital. 18% will benefit from cashless government schemes that pay for the procedures. An unpublished costing study conducted by a leading business school, found that Karnataka schemes pay only between 30% and 60% of the actual costs incurred by private hospitals. The chart below shows the discrepancy for surgical oncology.
So how does it make sense to operate on a large chunk of patients at well-below operating costs? Cross-subsidization. Hospitals use the margins from private rooms and complex surgeries to pay for patients who can’t afford surgeries. This is classic price discrimination and it works to everyone’s benefit. The rich get a better room and faster service, and the poor get an operation they couldn’t otherwise afford. Now what happens when you control all the prices in a hospital? Let’s also assume that hospitals will no longer make any profits[7] but will be paid an equilibrium price that accounts for actual costs incurred. In this alternate reality, a farmer from Mandya and Vijay Mallya might pull into my hospital for the same operation. The farmer would end up paying well over what he could afford, and Vijay Mallya will have to stay in the general ward but will get a great deal on his operation. The farmer has subsidized the tycoon and nobody is happy.
To conclude, India has the most vibrant free market for healthcare services in the world. A free market spawns intense competition, that’s why the Indian healthcare sector has grown at double digits and reduced the cost of medical procedures to the lowest in the world[8]. Indian hospitals have pioneered process innovations like factory-line operating rooms, and minimally invasive surgeries that are the envy of the developed world. Healthcare is still unaffordable for most Indians, but this is because of extremely high input costs. Our real estate costs are high because not enough land is zoned for hospitals. Our specialists are paid tremendous salaries because we produce a large number of doctors and an insignificant number of specialists. Medical equipment is imported at dollar prices because there isn’t a large enough market for equipment manufacturers to make in India. This doesn’t grab headlines the way, “Hospitals cheat patients” does, but anyone who spends ten minutes on a root-cause analysis will come to the same conclusions that I’ve outlined. There is a proper role for regulation, and it is to create an enabling environment for market forces to move in the direction that benefits the most people. It will be a tragedy to reverse two decades of gains if the Karnataka government uses a short term fix to solve a long-term problem.
Reference:
[1] Section 1, The Karnataka Private Medical Establishments (Amendments) Bill, 2017
[2] Section 10(3), The Karnataka Private Medical Establishments (Amendments) Bill, 2017
[3] Section 19(4a), The Karnataka Private Medical Establishments (Amendments) Bill, 2017
[4] Peforming Arts: The Economic Dilemma, 1966
[5] National Accreditation Body for Hospitals and Healthcare Providers
[6] But if you’re interested, please read this excellent summary – The Problems of Price Controls, from the Cato Institute
[7] The average PAT for Indian healthcare industry is around 4%. This isn’t a profitable business
[8] WHO, McKinsey, Harvard, take your pick. Everyone agree with this